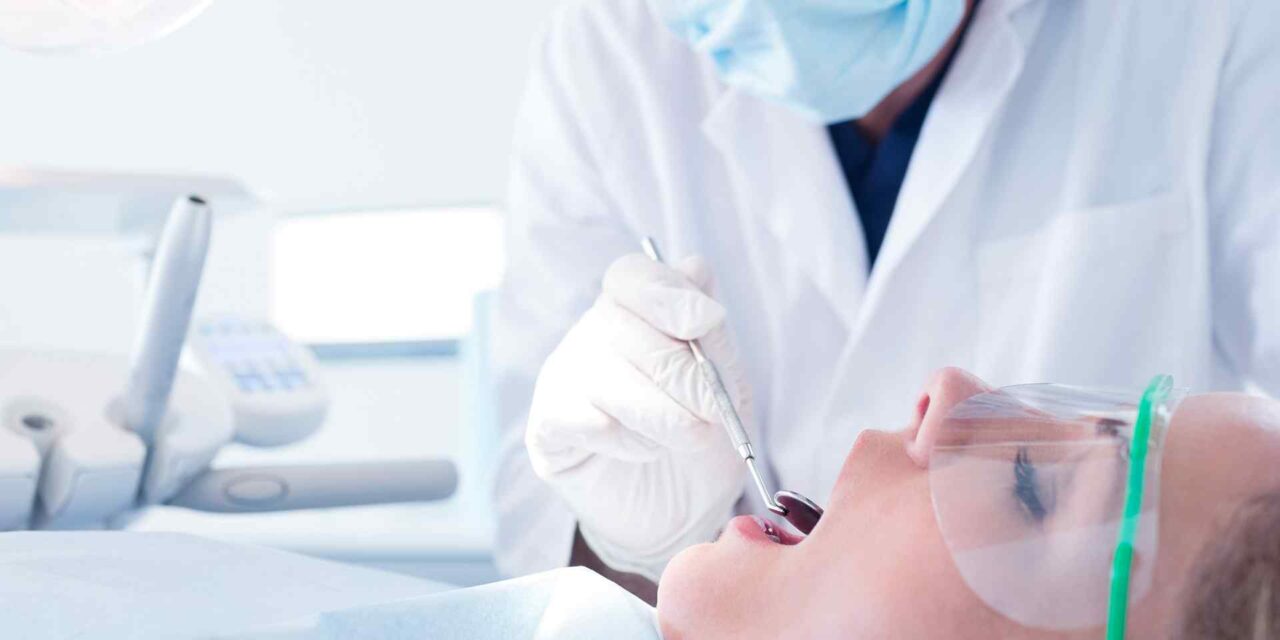
New research introduces a revolutionary treatment for these infections. The group is utilizing electrochemical therapy (ECT) to enhance the ability of antibiotics to eradicate the microbes.



New research introduces a revolutionary treatment for these infections. The group is utilizing electrochemical therapy (ECT) to enhance the ability of antibiotics to eradicate the microbes.

Brushing teeth frequently is linked with lower risks of atrial fibrillation and heart failure, according to a study published today in the European Journal of Preventive Cardiology, a journal of the European Society of Cardiology (ESC).
Teeth constitute a permanent and faithful biological archive of the entirety of the individual's life, from tooth formation to death, a team of researchers has found. Its work provides new evidence of the impact that events, such as reproduction and imprisonment, have on an organism.
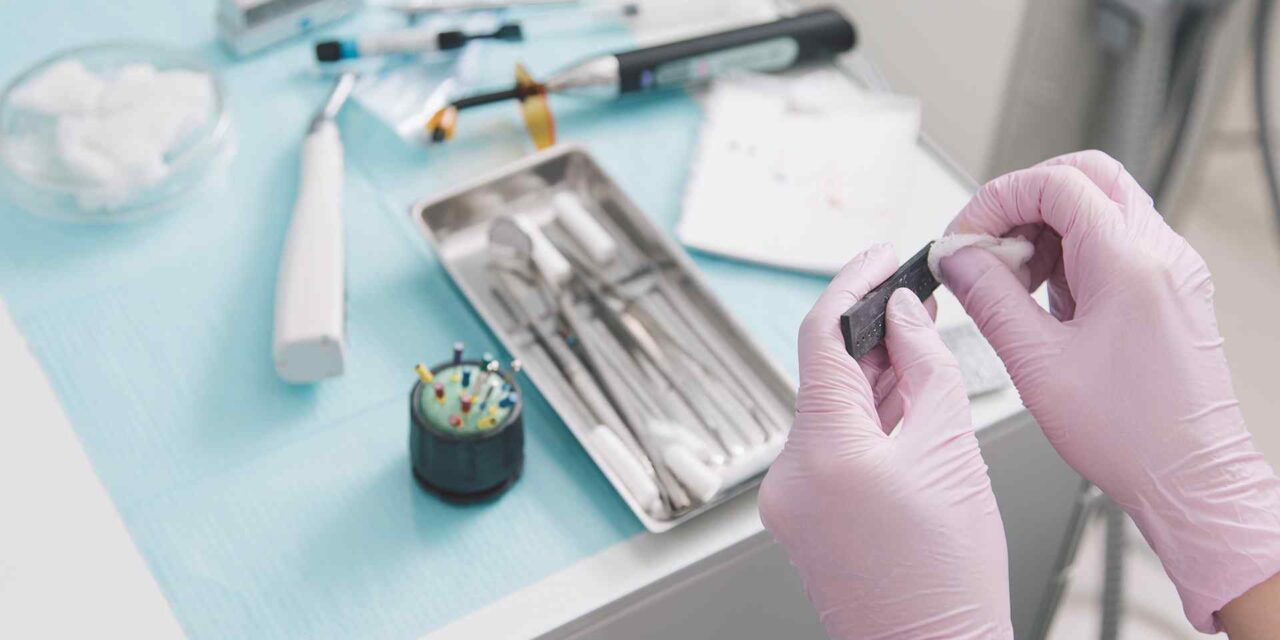
The use of opioids to soothe the pain of a pulled tooth could be drastically reduced or eliminated altogether from dentistry, say University of Michigan researchers.
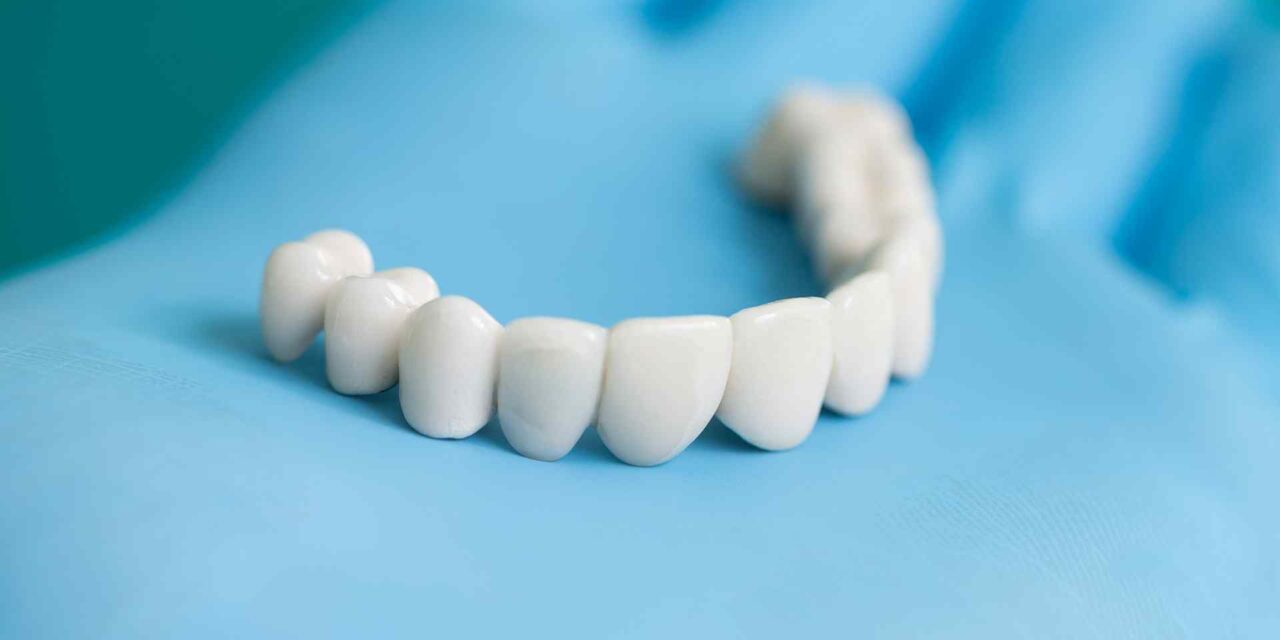
A dental bridge replaces one or more missing or broken teeth with fake teeth. Bridges use one or more real teeth on either side of the gap to hold the fake teeth in place.
Glossitis is typically characterized by an inflammation of the tongue. It can also cause changes in the tongue's texture and color.
A tooth infection, or an abscessed tooth, generally occurs as a result of tooth decay and poor oral hygiene. However, it can also develop due to previous dental work or traumatic injury.
When a person has a cavity in their tooth, a dentist will probably recommend a filling. Fillings are safe and effective, but some people might experience discomfort or tooth sensitivity afterward.
The soft palate is the muscular part at the back of the roof of the mouth. It sits behind the hard palate, which is the bony part of the roof of the mouth. The palates play important roles in swallowing, breathing, and speech.
Fluoride is a naturally occurring mineral that helps build strong teeth and prevent cavities. For more than 70 years, most of the tap water in America has contained small amounts of fluoride to reduce tooth decay.